The fields of public health, demography, health services research, and clinical practice have long relied on the paradigm of pregnancy intentions and “unintended pregnancy” as a key metric of reproductive health and wellbeing. However, this framework is fraught with limitations: it fails to reflect the lived experience of many people for whom “planning” a pregnancy is not desired or possible, excludes abortion or adoption as legitimate ways of navigating pregnancy, and largely ignores the structural conditions (e.g., poverty, racism, access to reproductive healthcare) that shape reproductive possibilities. Researchers, practitioners, and advocates have called for new, rigorously-developed paradigms to address these limitations.
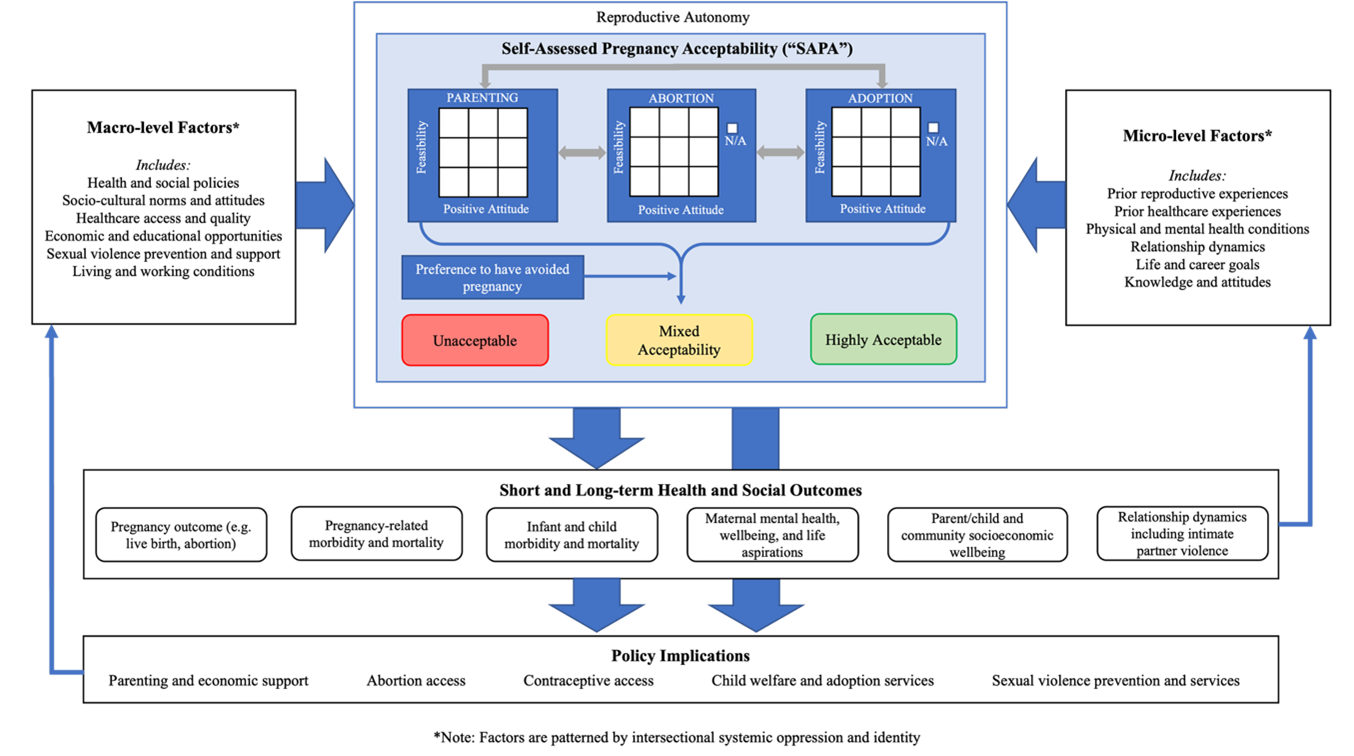
Our research team responded to these calls by working with diverse stakeholders to develop a novel framework and measure: self-assessed pregnancy acceptability (SAPA, see Figure 1). We define SAPA as a retrospective epidemiological measure capturing a person’s initial self-assessment upon learning they are pregnant—specifically their attitude toward and perceived feasibility of the potential pathways through the pregnancy (i.e., parenting, abortion, adoption)—in the context of their life circumstances. In our new Studies in Family Planning paper, “Moving Beyond Unintended Pregnancy: Development of a Person-Centered Conceptual Framework and Measure of Self-Assessed Pregnancy Acceptability,” we highlight four major advances this framework and measure can contribute to our field.
First, unlike unintended pregnancy (which was developed by researchers without rigorous stakeholder engagement), our framework centers on the lived experiences of diverse pregnant people through in-depth interviews, an expert panel including people with recent lived experience of pregnancy, and cognitive interviews with pregnant people.
Second, the SAPA framework and measure comprises all three possible pathways through pregnancy: parenting, abortion, and adoption (broadly defined as formal or informal including surrendering the baby).
Third, each pathway is characterized along two dimensions: one’s personal attitudes about that pathway for this pregnancy (positive, mixed, or negative) and one’s self-assessed feasibility of pursuing that pathway (high, mixed, or low). In this way, SAPA integrates the structural conditions that contextualize pregnancy including the resources they have for parenting and their access to abortion care. A given pathway is considered “open” to the individual if they have positive attitudes about the pathway (e.g., parenting is the right option) and perceive that it is highly feasible (e.g., I have enough resources to parent). A pathway is considered “closed” if attitudes toward it are negative or feasibility is low.
Fourth, SAPA is designed to generate directly actionable policy and clinical insights beyond the limited scope of contraceptive policy that is the current focus of pregnancy planning approaches. The SAPA measure does identify the proportion of individuals who preferred not to get pregnant but lacked the resources to prevent pregnancy, so it still informs contraceptive policy and access strategies. But it goes further. SAPA also quantifies the proportion of pregnancies that are not highly acceptable because individuals lack the material resources to parent or lack access to abortion care. And while very few people in the validation study report considering adoption (~3%), SAPA does ask if people have the information and resources needed to pursue adoption. This data point can signal potential unmet need for child welfare and adoption services. Finally, by asking about sexual coercion, the SAPA measure is able to estimate the proportion of pregnancies resulting from violence and inform violence prevention and social service needs.
The SAPA measure is currently being evaluated in a national validation study with 600 pregnant individuals. Preliminary results suggest strong convergent and predictive validity with established measures of reproductive health and wellbeing. While no single measure can perfectly reflect the wide array of pregnancy experiences and circumstances, the SAPA framework and survey items are person-centered, developed with diverse stakeholders, inclusive of abortion and adoption, structurally-informed, and relevant to reproductive policy and practice beyond contraception. Together, they offer an important conceptual and empirical shift in the fields of public health, demography, and sexual and reproductive health, moving away from the longstanding and limited unintended pregnancy paradigm and towards approaches that more accurately reflect lived experiences and support reproductive autonomy.
Figure 1. Conceptual model of self-assessed pregnancy acceptability (SAPA)